Phone Appointment
[smartblock id=45]WhatsApp Appointment
[smartblock id=46]Breast cancer is the most common type of cancer among women in Singapore today. 1 out of every 16 women in Singapore is likely to be afflicted by breast cancer, with more than 1,300 new cases diagnosed every year.

Normal cells divide and reproduce in an orderly manner. Your body relies on this orderly activity to repair injuries and replace worn-out tissue. Sometimes this orderly process is disrupted. Cells grow and divide out of control, producing extra tissue to form a mass or lump called a tumour. A tumour can be benign or malignant.
Benign tumours are not cancers. They may grow slowly but do not spread to other parts of the body.
Malignant tumours are cancerous growths and have the potential to spread to other parts of the body.
Breast cancer is a malignant tumour which occurs when breast cells become abnormal and divide without control or order. The majority of breast cancers start in the milk ducts. A small number start in the milk sacs or lobules. Within these two groups, some grow very slowly while others develop more rapidly. Breast cancer can spread to the lymph nodes and to other parts of the body such as the bones, liver, lung and sometimes to the brain.
The causes of breast cancer are not exactly known but there are risk factors that increase the chance of developing breast cancer. Having risk factors does not mean a woman will definitely develop breast cancer, as many women who have had breast cancer did not have any apparent risk factors. Some risk factors such as gender and age, or those related to our environment cannot be changed (non-modifiable), while others are modifiable as they are related to our lifestyle choices.
Non-modifiable Risk Factors
- Age and gender
- Early menarche, late menopause
- Family history and genetic factors
- Previous breast cancer
- Certain breast changes in biopsies (such as atypical ductal hyperplasia and LCIS)
- Radiation exposure for medical Reasons
Being a woman is a risk factor for developing breast cancer. Women have a much higher chance of developing breast cancer than men due to the female hormones oestrogen and progesterone. This risk is increased with longer hormonal exposure in women with early menarche (onset of menstruation) before the age of 12 and late menopause (after the age of 55).
Exercise will help reduce your risk of breast cancer. Usage of oral contraceptive pills and combined hormonal replacement therapy is a modifiable risk factor for breast cancer.
Other hormonal-related factors include never having children, late childbearing (after the age of 30), and obesity, especially excessive weight gain in post-menopausal women. This risk also increases with age.
Genetic factors and family history of breast cancer, especially in a first-degree relative (mother, sister or daughter), or two or more close relatives such as cousins and the presence of genetic alterations in certain genes such as BRCA1 and BRCA2 are associated with significant lifetime risks of breast cancer.
A past history of breast cancer, radiation exposure for medical reasons and certain benign conditions such as atypical ductal hyperplasia, atypical lobular hyperplasia or lobular carcinoma in-situ diagnosed on breast biopsy also increase the risk.
Modifiable Risk Factors
- Lack of exercise
- Excessive alcohol consumption over a long period of time
- Smoking
- Use of oral contraceptive pills (OCP) and combined hormonal replacement therapy (HRT) over a long period of time.
However, most women who have breast cancer have none of the above risk factors. Likewise, not possessing any of these risk factors does not mean that one will not get breast cancer. There are ongoing researches to learn more about these factors, as well as ways to prevent breast cancer.
Reducing the Risk of Breast Cancer
There is no sure way to prevent breast cancer, but the risks can be lowered.
These include modifying the risk factors which we have control over such as:
- Exercise and increasing physical activity
- Limiting alcohol intake
- Keeping a healthy diet to prevent obesity, especially post-menopause
- Cease smoking. Smoking increases the risk of many other cancers and is bad for overall health and there are suggestions of links between smoking and breast cancer
- Have more children if one is able to
- Breastfeeding is also protective
- Limit the use of HRT and OCP
- Limit the exposure to environmental pollution and radiation such as the use of medical imaging like computerised tomography (CT) scans unless really necessary
In high-risk women, such as those with a very strong family history or have genetic mutations such as the BRCA, risk-reducing options include taking drugs or having surgery that can reduce their risk. Risk-reducing surgeries include removal of the breast (mastectomy) and removal of the ovaries.
An alternative management strategy to risk-reduction methods is close surveillance. While this does not reduce the risk of cancer development, it does improve outcome by discovering the cancers in earlier stages, allowing earlier treatment and hence better outcomes.
Breast cancer can be classified by the stage of cancer at diagnosis and their biological characteristics. These will determine treatment recommendations as it has prognostic (most likely outcome of the disease) implications and treatment implications.
Staging
Understanding the stage of the cancer is important to understand the prognosis and the treatment recommendation.
Cancers treated in earlier stages have better outcomes, more advanced cancers will need more aggressive treatment.
Cancer stage is based on:
- Whether the cancer is non-invasive or invasive
- The size of the invasive cancer
- Whether the cancer has spread to the lymph nodes
- Whether the cancer has spread to other parts of the body
The TNM staging system is based on:
T: Size of the tumour
N: Lymph node involvement
M: Metastasis when cancer has spread to other organs like the lung, liver and bones.
Different T, N and M in combination will determine the stage of the cancer.
Stage 0 or Ductal Carcinoma in Situ (DCIS) is a common non-invasive breast cancer, where cancer cells are still within the ducts and have not grown out to breach the duct linings into the surrounding normal breast tissue.
DCIS, also known as Stage 0 breast cancer, unlike invasive breast cancer, is not life-threatening, but it can increase the risk of developing an invasive breast cancer.
lnvasive breast cancer occurs when cancer cells spread beyond the ducts or lobules resulting in invasive ductal and invasive lobular breast cancer, the two most common subtypes of breast cancer.
Metastatic breast cancer refers to the stage when the cancer has spread beyond the breast to distant organs such as the lungs, liver or bones.
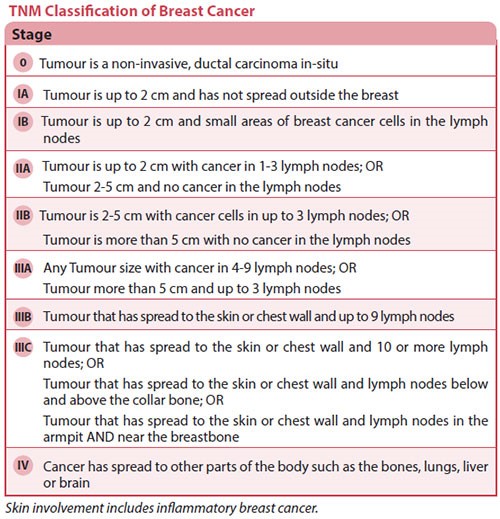
TNM Classifications of Breast Cancer
Tumour Biology
Breast cancers are also differentiated by the presence of special receptors on the surface of the cancer cells, such as the:
- Oestrogen receptor
- Progesterone receptor
- HER2 (Human Epidermal Growth Factor 2) receptor
This is associated with the aggressiveness of the cancer and affects the prognosis of the patient.
More importantly, there are drugs to target these changes, and hence directed treatment for them will improve the outcome.
The histopathological (microscopic appearance) subtype of the cancer also helps to determine the prognosis, and nature of breast cancer overall.
The grade (assessment of how abnormal the cancer cells look) also determines the aggressiveness and hence, treatment recommendations.
The most common subtype is the invasive carcinoma of no special type (NST). Specific subtypes include invasive lobular, tubular, cribriform, metaplastic, apocrine, mucinous, papillary and micropapillary carcinoma, as well as carcinoma with medullary and neuroendocrine (WHO classification 2012).
If there is an unusual lump or changes in the breasts, seek medical attention. Try to pinpoint the area accurately as this will assist the doctor with the examination. Tests will be recommended to obtain a definite diagnosis.
Imaging
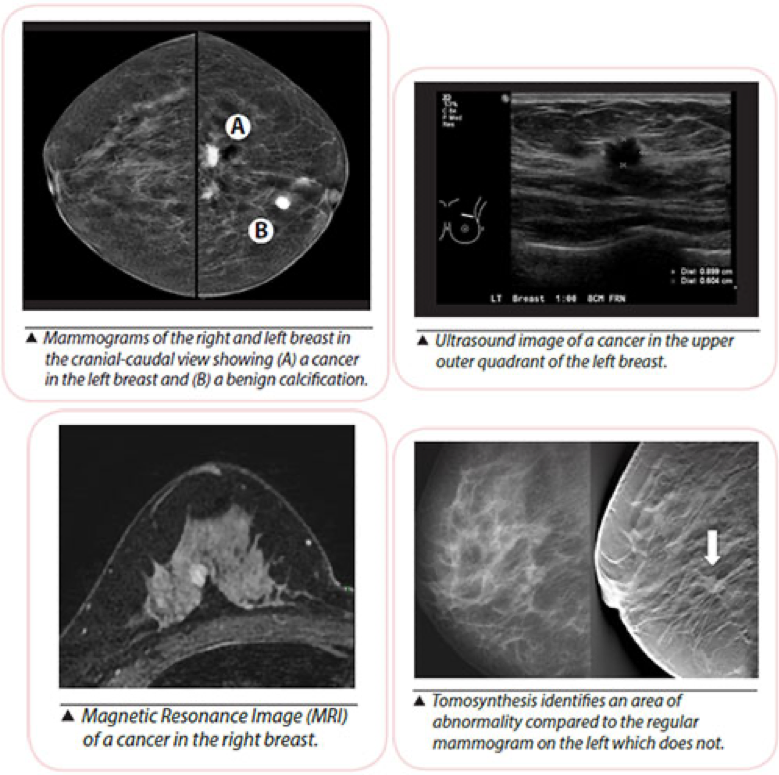
Mammogram
Mammography is a low-powered X-ray technique that gives a picture of the internal structure of the breast. Usual screening mammograms involve taking X-ray images of the breast compressed between two plates with two views taken — cranial caudal or horizontal and mediolateral oblique or diagonal.
Additional angles and magnified views may be taken if there are areas of concern. It can detect the presence and position of the abnormalities and help in the diagnosis of breast problems, including cancer.
Any previous mammograms (and reports if available) should be brought along when seeing a doctor.
Sometimes a lump that can be felt is not seen on a mammogram. Other tests may be necessary to determine if the lump is cancerous.
Ultrasound
Breast ultrasound is the use of high- frequency sound waves to produce an image of breast tissue.
The sound waves are transmitted from the probe through the gel into the body. The transducer collects the sounds that bounce back and a computer then uses those sound waves to create an image.
Magnetic Resonance lmaging (MRI)
This uses a combination of magnetism and radio waves to build up a picture consisting of detailed cross-sections of pictures of the breasts.
The test involves lying on the stomach on a padded platform, with cushioned openings for the breasts, that passes through a tunnel-like structure (which forms a very large magnet). It may take up to one hour to complete, but is completely painless.
MRI is useful when mammograms are not suitable, e.g. in young women with dense breast tissue or when findings on mammograms and ultrasound are not conclusive to achieve a diagnosis.
It is used as a screening tool for young women with high-risk factors like BRCA gene carriers or those with a very strong family history of breast cancer.
Tomosynthesis
This involves taking multiple X-rays of each breast from many angles. The breast is positioned the same way as in a conventional mammogram, but only a little pressure is applied, just enough to keep the breast in a stable position during the procedure.
An X-ray tube moves in an arc around the breast while images are taken. Information is sent to a computer, where it is assembled to produce clear, highly-focussed 3-dimensional images throughout the breast.
Biopsy
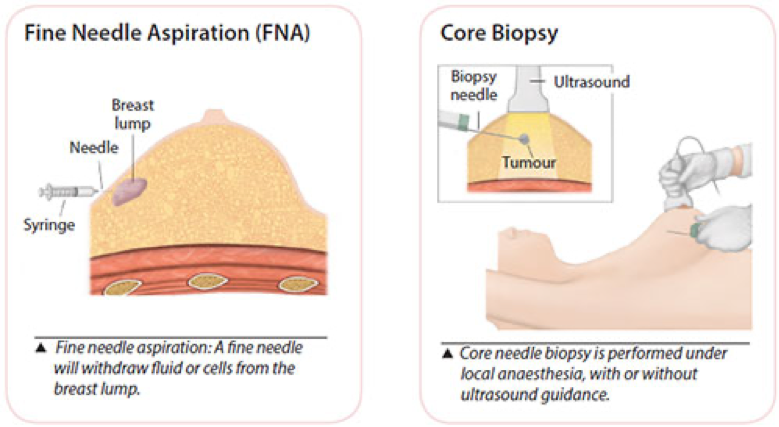
Fine Needle Aspiration (FNA)
A syringe with a very fine needle is used to withdraw fluid or cells from a breast lump. This is a simple procedure and can be uncomfortable but is usually tolerable enough for it to be done in the clinic.
If the lump is just a cyst, withdrawing fluid in this manner will usually make the cyst disappear.
However, if the lump is solid, your doctor may use this procedure to withdraw some cells from it. The cells will then be sent to a laboratory for examination.
Core Needle Biopsy
This is a minimally invasive method that obtains a few tiny strips of tissue from an area of abnormality with a wide bore needle. Local anaesthetic is injected to numb the breast area, followed by a small incision in the skin to allow easy insertion of the needle.
If the abnormality is non-palpable (not detectable by clinical examination) and visible on the ultrasound, ultrasound guidance is used to obtain the tissue. Usually 2 to 6 cores of tissue will be obtained for examination.
A nurse will apply compression to the breast to stop any bleeding. The wound is closed by a steristrip and the dressing applied. Strenuous activity is to be avoided for 2 days after the biopsy.
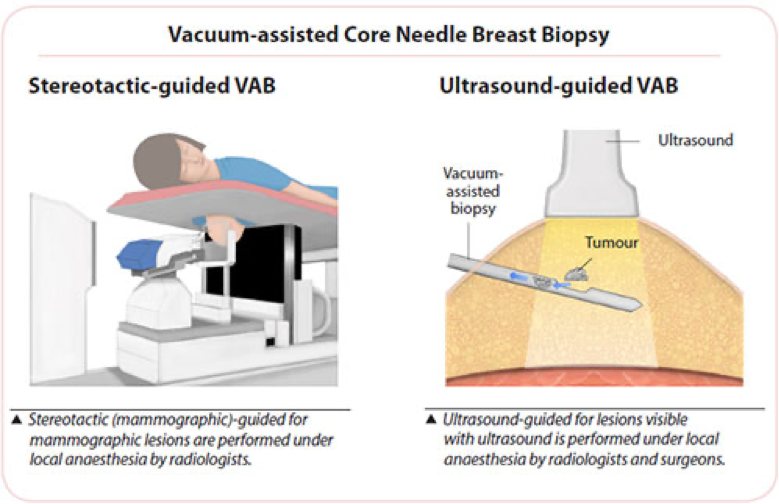
Vacuum-assisted Core Needle Breast Biopsy
Vacuum-assisted biopsy (VAB) devices use a larger bore needle with a vacuum component to obtain tissue samples from non-palpable lesions.
Like the usual core biopsy, this minimally invasive procedure is also performed under local anaesthesia, which is injected to numb the breast area, followed by a small incision in the skin to allow easy insertion of the needle. It is used for lesions seen by mammography (stereotactic-guided biopsy), ultrasound or MRI.
The surgeon or radiologist places the probe into the suspicious area of the breast accurately. A vacuum then draws the tissue into the probe, a cutting device removes the tissue sample and then carries it through the probe into a collection area.
More tissue is usually obtained using the VAB than the usual core needle biopsy and the number of strips removed is dependent on the area that needs to be examined.
A small titanium clip (microclip) may be placed at the biopsy site as a location marker for future treatment. This clip is very small (2 mm), is harmless, and will not cause any problems when left inside the breast. An X-ray is taken post-biopsy to ensure proper clip placement. New biodegradable markers are also available now.
A nurse will apply compression to the breast to stop any bleeding, the wound is closed by a steristrip and the dressing applied. Strenuous activity is to be avoided for 2 days after the biopsy.
This procedure is minimally invasive as compared to an open surgical biopsy. It is performed as a day surgery procedure. lt has the ability to sample tiny abnormalities called microcalcifications, making early diagnosis of breast cancer possible.
Under local anaesthesia, it takes about 30 to 45 minutes to complete. The procedure is usually not painful but you may experience some discomfort.
Excision Biopsy
An excision biopsy is the removal of a lump or sample of suspicious tissue by surgery for examination under a microscope to give a definite diagnosis.
For lesions that are small or not palpable, accurate marking of the area for surgery is necessary. These include using ultrasound during surgery, or with procedures done just before surgery to mark the area to be operated.
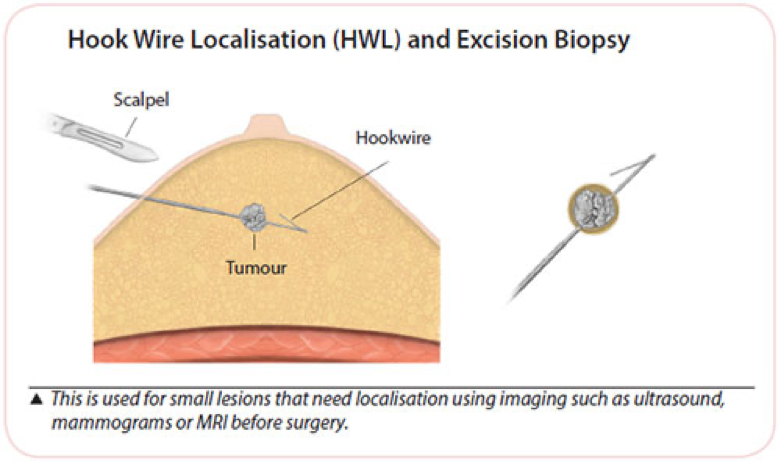
Ultrasound, mammogram or MRI can be used to insert a small thin wire to the abnormal spot in the breast.
This wire is used to guide the surgeon to remove the area accurately. This technique is known as Hook Wire Localisation (HWL) Biopsy.
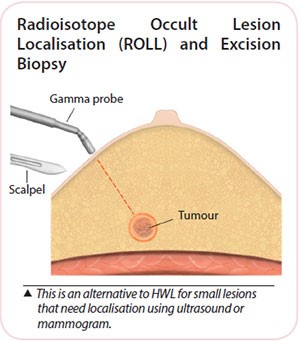 An alternative method known as Radioisotope Occult Lesion Localisation (ROLL) uses a small amount of radioactive substance injected into the lesion. This area is detected with a radioactive sensor used during surgery that allows the lesion to be accurately removed.
An alternative method known as Radioisotope Occult Lesion Localisation (ROLL) uses a small amount of radioactive substance injected into the lesion. This area is detected with a radioactive sensor used during surgery that allows the lesion to be accurately removed.
This technique does not have the discomfort of the hookwire and the need to perform mammograms after the wire placement to check their positions.
Excision biopsies are often performed under general anaesthesia, depending on the size and position of the lump, but local anaesthesia may be used for small lesions close to the skin.
As a minor day surgery procedure, patients can return home after surgery. Strenuous activity is to be avoided for the first few days; immediate ability for usual light activities of daily living is expected.
Post-operative advice may differ between individuals depending on their needs and circumstances. In general, most will be able to return to work in a week.
Treatment of breast cancer often involves more than one therapy, and may be a combination of therapies.
Treatment recommendations depend on factors such as the cancer type, stage of the cancer, size of the tumour in relation to the breast size, whether breast preservation is desired and the patient’s general health.
Personal preferences determine certain choices, if the option is available, such as the options for the type of surgery. Being diagnosed with breast cancer and having to decide on the treatment options may be difficult. The support of friends and family during the consult and discussion on the results of tests and treatment is recommended.
Local and Systemic Therapy
- Local therapy includes surgery and radiotherapy. It treats the cancer at the site e.g. the breast and axilla (armpit) without affecting the rest of the body.
- Systemic therapy refers to the use of drugs which enter the bloodstream to reach the rest of the body, targeting cancer cells anywhere in the body. Chemotherapy, hormone therapy, and targeted therapy are systemic therapies.
In early breast cancer, surgery is the first treatment of choice. Chemotherapy, targeted and hormonal therapy may be used before surgery (neoadjuvant therapy), or after surgery (adjuvant therapy). Radiotherapy is usually given after surgery.
In stage IV cancer, the goal is to stabilise the disease with systemic therapy. However, local treatment of tumours with radiation therapy or surgery may be recommended when symptoms need to be alleviated.
The two broad options are breast-conserving surgery (BCS) or mastectomy.
Breast-Conserving Surgery (BCS)
Wide Excision Breast-Conserving Surgery
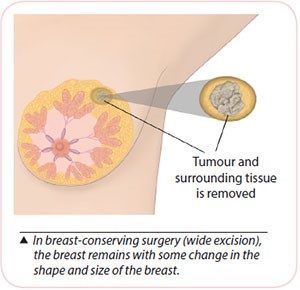 In this surgery, the breast cancer and a rim of normal surrounding breast tissue are removed. The breast will remain; a scar and some changes in shape and size of the breast are expected. Patients can go home on the same day or the next day.
In this surgery, the breast cancer and a rim of normal surrounding breast tissue are removed. The breast will remain; a scar and some changes in shape and size of the breast are expected. Patients can go home on the same day or the next day.
After recovering from breast-conserving surgery, radiation therapy to the breast (Mon to Fri) for 3 to 6 weeks is recommended. It helps to reduce the risk of recurrence.
A second operation is needed if cancer cells are noted at the edge in the histological (microscopic) assessment of the removed portion. This occurs in 10 to 15 percent of patients.
Oncoplastic Breast-Conserving Surgery
In some patients undergoing breast-conserving surgery, additional procedures may be recommended to prevent severe deformities of the breast.
Breast-Conserving Surgery with Mammoplasty (Reshaping with Breast Uplift / Breast Reduction)
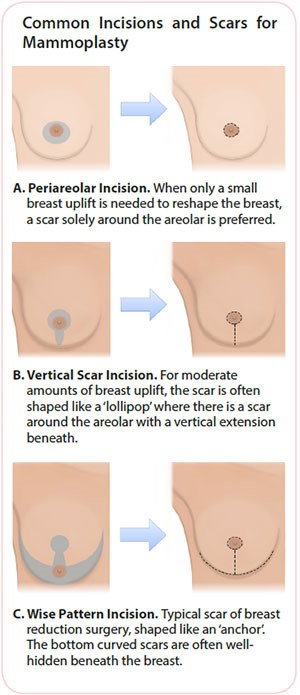 To avoid significant breast deformity after breast-conserving surgery (wide excision), breast reshaping (mammoplasty) may be performed. This is possible if the patient has sufficient remaining breast volume, and often takes the form of a breast uplift or breast reduction. Excess skin may need to be removed, and the exact scar depends on the size of cancer removed and the patient’s existing breast shape.
To avoid significant breast deformity after breast-conserving surgery (wide excision), breast reshaping (mammoplasty) may be performed. This is possible if the patient has sufficient remaining breast volume, and often takes the form of a breast uplift or breast reduction. Excess skin may need to be removed, and the exact scar depends on the size of cancer removed and the patient’s existing breast shape.
The most common scars are illustrated (right). If a large reduction is needed, and significant asymmetry in breast volume is anticipated, surgery to the opposite breast may be performed to improve final breast symmetry. This may be performed at the same surgery or as a delayed procedure after cancer treatment.
Partial Breast Reconstruction – Volume Replacement with a Local Perforator Flap
Fatty tissue next to (or below) the breast is used to fill the space in the breast as a result of cancer removal. This maintains breast volume and contour, maintains the nipple position and greatly reduces breast deformity.
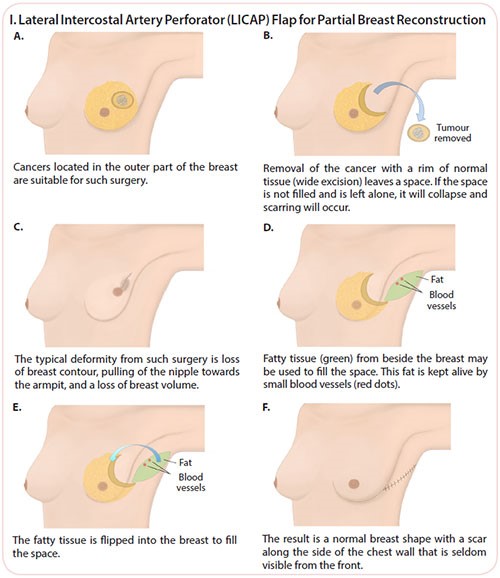
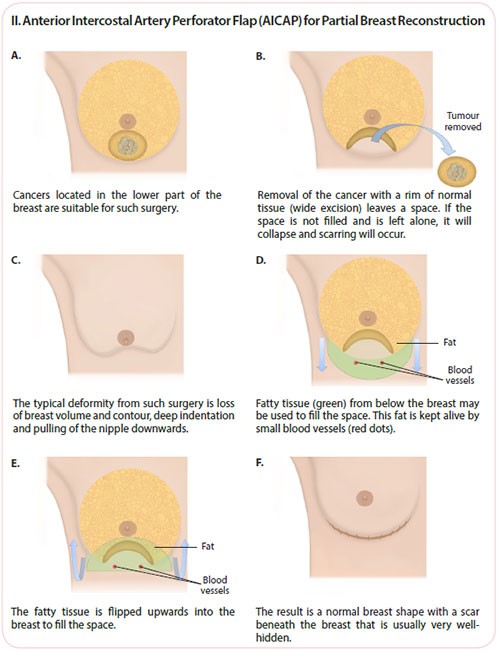
Image-Guided Localisation for Surgery
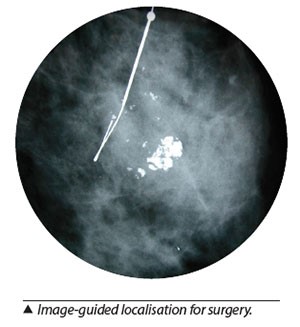 For non-palpable tumours that need to be removed with surgery, localisation with a hookwire or a localising substance under image guidance done prior to the surgery is needed.
For non-palpable tumours that need to be removed with surgery, localisation with a hookwire or a localising substance under image guidance done prior to the surgery is needed.
This procedure is performed under local anaesthesia, prior to surgery. Mammogram, ultrasound or MRI guidance is used to accurately locate the site for surgery.
A fine wire (hookwire) is inserted or a radioactive substance is injected into the breast, within or in close proximity to the lesion of interest, which will be removed during the surgery.
Mastectomy
Mastectomy is the removal of the whole breast (incorporating the breast tumour). In general, there are two types of mastectomy:
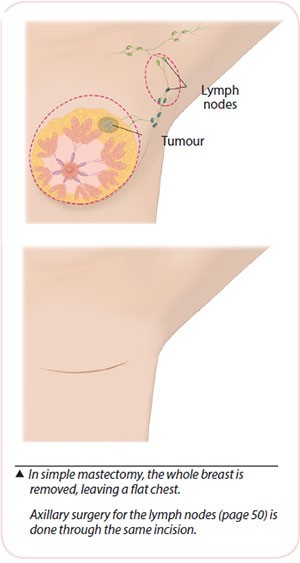
Simple Mastectomy
In a simple mastectomy, the breast, including the nipple-areola complex is removed. After surgery, the chest is flat, with a scar across it. A drain, which is a soft tube, is placed during surgery with the accompanying bottle to remove blood and tissue fluid accumulated at the operated site.
The drain will be removed when the drainage is less than 30 ml a day after 1 to 2 weeks. Drain and wound care will be taught to patients and their caregivers before discharge and patients can go home the next day.
Mastectomy with Whole Breast Reconstruction
Breast reconstruction is surgery to ‘recreate’ a breast using one’s own body tissue or implant after mastectomy. It provides the breast shape, but has no natural feeling.
Immediate breast reconstruction is when reconstruction is done at the time of mastectomy.
Skin-sparing mastectomy is where most of the skin of the breast will be preserved.
Nipple-sparing mastectomy is considered for suitable cases, where the nipple may be preserved if tissue from the base of the nipple shows no cancer cells when tested at the time of surgery. However, if the final histology results show cancer cells behind the nipple, a simple surgery to remove the nipple will be recommended.
Delayed breast reconstruction may also be done at a later stage, separate from the initial breast surgery.
Types of Post-Mastectomy Reconstructions
Flap reconstructions
Skin, fat and sometimes muscle (a flap) from another part of your body may be used to make into a breast shape. This operation takes about 6 to 8 hours and requires a hospital stay of between 1 to 2 weeks. Several drains are used and removed after 1 to 2 weeks. Flaps may be from the following areas:
- Back (latissimus dorsi)
- Buttock
- Thigh
- Abdomen
- TRAM (transverse rectus abdominis myocutaneous) flap
- DIEP (deep inferior epigastric perforator) flap, taking skin and fat only
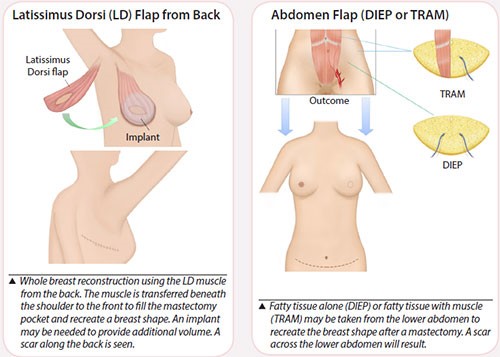
Additional procedures to improve the look of the breast after the initial surgery may include adding a nipple, surgery to the opposite breast to create a good match, or refining the shape of the recreated breast.
Breast implants
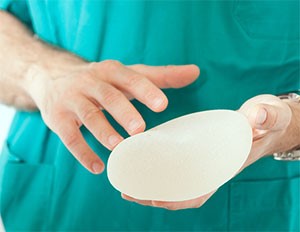
Silicone implants may be used to create a new breast and the operation takes about 4 to 5 hours. There are usually 2 to 3 drains inserted and the hospital stay is 2 to 5 days.
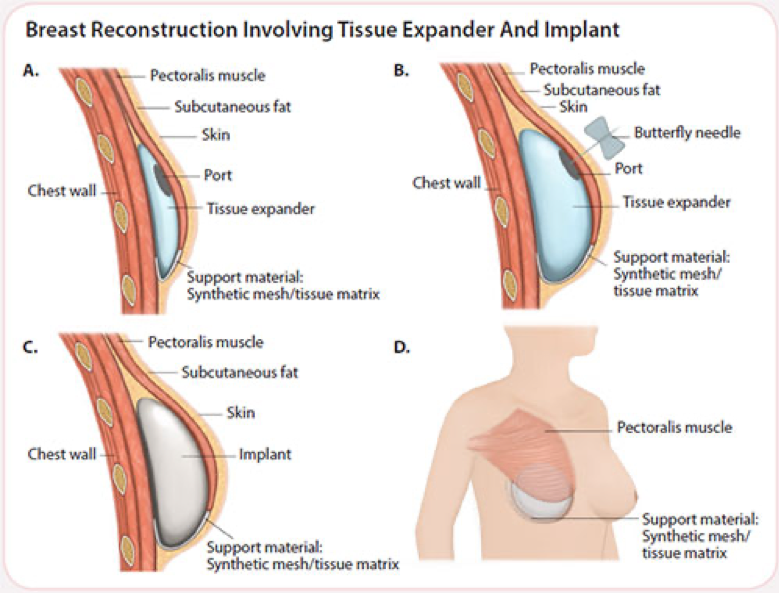
A 1-stage procedure is when the permanent implant is inserted at the time of mastectomy. A 2-stage procedure is when a temporary expander is placed at the time of mastectomy and gradually expanded to stretch the skin. The expander will be exchanged for a permanent implant at a later surgery.
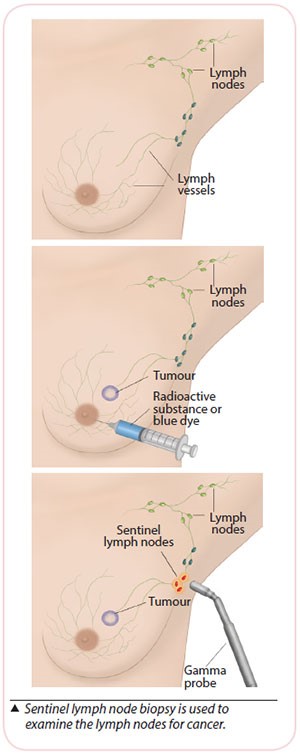 Sentinel Lymph Node Biopsy (SLNB) is recommended for early-stage breast cancer when the lymph nodes in the armpit do not appear to have cancer.
Sentinel Lymph Node Biopsy (SLNB) is recommended for early-stage breast cancer when the lymph nodes in the armpit do not appear to have cancer.
Sentinel lymph nodes (SLN) are the first few lymph nodes in the armpit where the lymphatic vessels from the breast drain to. These will be removed during surgery and examined under the microscope (frozen section) to determine if cancer has spread to the SLN.
This is done under general anaesthesia (GA). A blue dye or a radioactive substance is injected around the cancer site or at the nipple prior to surgery to locate the SLN. The radioactive substance will be injected before the operation. The blue dye will be injected during the operation.
If cancer is detected in the SLN, lymph nodes in the axilla will be removed. If no cancer is detected in the SLN, no further surgery is needed.
The final histology (microscopic assessment) will be reviewed about 1 week after surgery. In up to 5 percent of cases, the final assessment of the SLN may be different from the initial frozen section result and a second operation may be recommended.
If the dye or radioactive substance is not able to identify the SLN, removal of all the lymph nodes (axillary clearance) will be done.
Axillary clearance is the removal of all lymph nodes from the underarm when the lymph nodes are found to have cancer cells.
Side effects of axillary clearance include shoulder stiffness and numbness of the inner part of your upper arm. Lymphoedema (swelling of the arm) may occur in 10 to 15 percent of women. This is because lymph nodes drain fluid from the arm and their removal may cause fluid to accumulate in the arm on the operated side.
A separate axillary incision is often needed for patients undergoing breast conserving surgery.
High-energy rays are used to kill cancer cells or stop them from growing further.
Although radiation therapy can affect both cancer cells as well as normal cells, the aim of radiation is to destroy more cancer cells and spare as many normal cells as possible. Radiation therapy is given to the affected breast after a lumpectomy.
In some circumstances, it may be given to the chest wall after a mastectomy, or to the lymph nodes. It is usually given 5 days a week on weekdays, over a period of 3 to 6 weeks.
Radiation therapy can cause some side effects which vary among individuals.
Side Effects
The most common side effect is ‘sunburn’ on the skin, with redness and dryness of the skin observed.
The degree and intensity of the skin reaction is greater in patients receiving a large standard dose and in patients who have fair skin. Skin texture also becomes darker and thicker.
The breast may swell, and increase or decrease in insensitivity. Usually, these effects are temporary and are manageable.
Chemotherapy
This treatment uses anti-cancer drugs to prevent cancer cells from growing and reproducing themselves. These drugs are usually given by injection through veins into the blood stream to all parts of the body.
It is usually given over 3 to 6 months and may be used alone, before surgery (neoadjuvant) or after surgery (adjuvant) therapy, or together with targeted therapy to increase the effectiveness of the treatment, depending on the type and stage of cancer.
Chemotherapy is given in cycles. Each cycle consists of a treatment period followed by a resting (recovery) period. As cancer drugs also affect normal cells, the resting period is to allow the body to recover before the next treatment cycle starts.
Side Effects
There are side effects associated with chemotherapy such as hair loss, nausea and vomiting, loss of appetite, mouth ulcers and risk for infection. However, these are temporary and steps can be taken to prevent or reduce them.
Targeted Therapy
Breast cancers are also tested for special receptors. One such receptor is the Human Epidermal Growth Factor 2 (HER2) receptor. This receptor is over-expressed in about 25 percent of all breast cancers; the presence needs to be confirmed by laboratory tests performed on the biopsy specimen before the treatment is given.
The aim of the treatment is to reduce and hopefully eliminate existing cancer cells in the human body while minimising side effects on normal cells.
Trastuzumab, also known as Herceptin®, targets the HER2 (Human Epidermal Growth Factor 2) receptors on cancer cells to prevent cell growth and division.
Herceptin® has been shown to prolong survival in breast cancer patients with early and advanced disease (Stage IV) when used in combination with chemotherapy.
Side Effects
Patients who receive trastuzumab may complain of infusion-related reactions such as fever and chills. Rarely, weakening of the heart muscles (also known as cardiomyopathy) has been observed in some patients.
An increasing number of targeted drugs are becoming available for the treatment of breast cancer, including Lapatinib (which targets HER2 and EGFR) and Bevacizumab (which targets a factor associated with new blood vessel formation in tumours.
Hormonal Therapy
 Breast cancers are tested for oestrogen receptors (ER) and progesterone receptors (PR) on their surfaces as such cancers can be stimulated by oestrogen or progesterone to grow.
Breast cancers are tested for oestrogen receptors (ER) and progesterone receptors (PR) on their surfaces as such cancers can be stimulated by oestrogen or progesterone to grow.
Hormonal therapy is aimed at blocking this effect. The drug recommended is dependent on the menopausal status of the women.
Hormonal therapy can cause some side effects, and they are dependent on the type of drug taken and can vary from one patient to another.
Tamoxifen
This drug blocks the action of oestrogen on the body but does not stop oestrogen from being produced. Tamoxifen may cause hot flashes, depression or mood swings, vaginal discharge or irritation, irregular menstrual periods and sometimes menopause.
Any unusual bleeding should be reported to the doctor. It is recommended for pre-menopausal women, but can be used in postmenopausal women.
Side Effects
Serious side effects from Tamoxifen are rare but Tamoxifen can cause the formation of blood clots in the veins, especially in the legs. In a very small number of women, Tamoxifen can cause cancer in the lining of the uterus.
You may be referred to a gynaecologist to evaluate any unusual bleeding.
Aromatase lnhibitors (AI)
For post-menopausal women, another group of drugs called aromatase inhibitors (AIs) is also used in breast cancer hormonal treatment. Aromatase inhibitors work by blocking an enzyme called aromatase that the body uses to produce oestrogen.
The current Als such as anastrozole, letrozole and exemastane, are welltolerated and are used in the treatment of early stage and advanced breast cancer.
Side Effects
Side effects of AI include hot flashes, mood changes, nausea, vaginal dryness, joint pain/stiffness, tiredness, lethargy and osteoporosis (including a higher risk of fractures compared to Tamoxifen).
Regular follow up by the doctor after treatment is recommended due to the risk of developing breast cancer again.
This will include physical examination of the chest, underarms, neck, and the other breast with periodic mammograms.
Changes to look out for include:
- Changes in the surgical scar and treated area
- Any unusual changes in the treated or other breast
- Swollen lymph glands
- Bone pain
- Persistent cough
- Difficulty in breathing
- Jaundice